Few experiences are as emotionally painful and confusing as losing a pregnancy — especially when it happens more than once.
After two or more miscarriages, many couples begin asking difficult questions:
-
Why does this keep happening?
-
Is something wrong with my body?
-
Will we ever carry a pregnancy to term?
-
What treatments are available?
Recurrent pregnancy loss (RPL) is not just a medical condition. It is a deeply personal experience that affects emotional wellbeing, relationships, and future reproductive decisions.
The good news is this:
Many couples with recurrent pregnancy loss go on to have successful pregnancies — especially when the underlying cause is properly identified and treated.
This article explains what recurrent pregnancy loss means, why it happens, how it is investigated, and what fertility treatment options may help.
What Is Recurrent Pregnancy Loss?
Recurrent pregnancy loss is commonly defined as:
-
Two or more consecutive miscarriages, usually occurring in the first trimester (before 13 weeks of pregnancy).
Some guidelines define it as three or more losses, but many specialists begin evaluation after two.
RPL is different from infertility.
-
Infertility = difficulty getting pregnant.
-
Recurrent pregnancy loss = getting pregnant but not being able to maintain the pregnancy.
Both require evaluation, but the medical approach differs.
Why Does Recurrent Pregnancy Loss Happen?
Recurrent pregnancy loss is usually not caused by one single factor. It may involve:
-
genetic abnormalities
-
uterine structural issues
-
hormonal imbalances
-
immune system factors
-
blood clotting disorders
-
thyroid dysfunction
-
uncontrolled chronic medical conditions
-
lifestyle factors
-
male factors
-
unexplained causes
Understanding the cause is the foundation of effective treatment.
Step One: Proper Evaluation Before Treatment
Before starting any fertility treatment, a comprehensive evaluation is essential.
1. Genetic Testing
Genetic causes are among the most common reasons for early miscarriage.
Evaluation may include:
-
Karyotype testing for both partners (to detect chromosomal rearrangements)
-
Testing of pregnancy tissue from a miscarriage (if available)
Some couples carry balanced chromosomal rearrangements that do not affect them personally but increase the risk of miscarriage.
2. Uterine Assessment
Structural abnormalities inside the uterus can interfere with implantation and early development.
Tests may include:
-
Ultrasound
-
Saline infusion sonography
-
Hysteroscopy
-
MRI (in selected cases)
Common structural causes include:
-
uterine septum
-
fibroids inside the cavity
-
scar tissue (Asherman’s syndrome)
-
adhesions from previous surgery
3. Hormonal Evaluation
Hormonal imbalances can interfere with implantation and early pregnancy support.
Tests may assess:
-
Progesterone levels
-
Thyroid function (TSH, Free T4)
-
Prolactin
-
Insulin resistance (if PCOS is suspected)
Even mild thyroid dysfunction can increase miscarriage risk.
4. Blood Clotting and Immune Disorders
Certain clotting disorders increase the risk of miscarriage.
Testing may include screening for:
-
Antiphospholipid syndrome
-
Inherited thrombophilias
These conditions affect how blood flows to the placenta.
5. Male Factor Evaluation
Sperm health also influences embryo development.
Advanced sperm testing may evaluate:
-
DNA fragmentation
-
Morphology
-
Motility
High sperm DNA damage may increase miscarriage risk.
Fertility Treatment Options for Recurrent Pregnancy Loss
Treatment depends entirely on the cause.
There is no single universal treatment for RPL.
1. Genetic Causes: IVF with Preimplantation Genetic Testing (PGT)
If recurrent pregnancy loss is due to chromosomal abnormalities, treatment may include:
In Vitro Fertilization (IVF) with Preimplantation Genetic Testing (PGT).
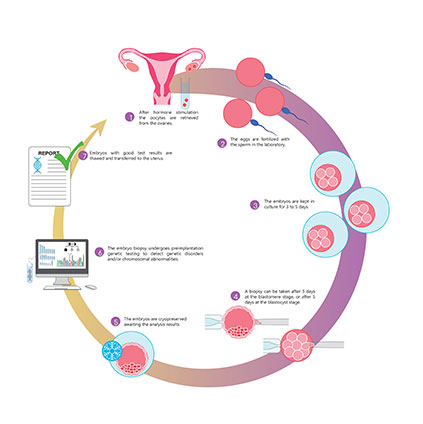
How it works:
-
Eggs are retrieved.
-
Fertilization occurs in the laboratory.
-
Embryos grow to the blastocyst stage.
-
A few cells are biopsied.
-
Embryos are genetically tested.
-
Only chromosomally normal embryos are transferred.
This reduces the risk of miscarriage caused by chromosomal errors.
It does not guarantee success, but it significantly improves the chances for couples with known genetic causes.
2. Uterine Structural Abnormalities: Surgical Correction
If imaging reveals structural abnormalities such as:
-
uterine septum
-
intrauterine scar tissue
-
certain fibroids
A minor surgical procedure (often hysteroscopic surgery) may be recommended.
Correcting structural defects can:
-
improve implantation
-
reduce miscarriage risk
-
restore normal uterine anatomy
Many women conceive successfully after correction.
3. Hormonal Support Therapy
If hormonal imbalance is identified, treatment may include:
Progesterone supplementation
Progesterone supports the uterine lining during early pregnancy.
Supplementation may be given:
-
after ovulation
-
or after embryo transfer
-
or once pregnancy is confirmed
This is common in women with suspected luteal phase issues.
Thyroid treatment
If thyroid dysfunction is detected:
-
Levothyroxine may be prescribed for hypothyroidism.
-
Levels are closely monitored before and during pregnancy.
Correct thyroid management significantly reduces miscarriage risk.
4. Treatment for Antiphospholipid Syndrome
If antiphospholipid syndrome is diagnosed, treatment typically includes:
-
Low-dose aspirin
-
Low molecular weight heparin (blood thinner injections)
This improves blood flow to the developing placenta and reduces clot formation.
This combination has helped many women carry pregnancies to term.
5. Managing PCOS and Insulin Resistance
In women with polycystic ovary syndrome (PCOS):
-
Insulin resistance
-
Hormonal imbalance
-
Poor egg quality
may contribute to miscarriage.
Treatment may include:
-
Lifestyle modifications
-
Weight optimization
-
Insulin-sensitizing medications
-
Ovulation induction when necessary
6. Lifestyle-Based Fertility Optimization
While not a standalone “treatment,” lifestyle optimisation plays a powerful supportive role.
Couples may be advised to:
-
Stop smoking
-
Reduce alcohol
-
Achieve healthy weight
-
Improve sleep quality
-
Reduce chronic stress
-
Optimize nutrition
Lifestyle does not cure structural or genetic problems, but it supports embryo development.
7. Treatment for High Sperm DNA Fragmentation
If male testing shows high DNA fragmentation, strategies may include:
-
Antioxidant therapy
-
Lifestyle modifications
-
Treating underlying infection or varicocele
-
Using advanced sperm selection techniques in IVF
Sperm quality affects embryo stability more than many couples realise.
8. Expectant Management (When No Cause Is Found)
In some cases, all tests return normal.
This is called unexplained recurrent pregnancy loss.
Although this is frustrating, it is important to know:
Many couples with unexplained RPL still achieve a successful pregnancy naturally.
In such cases, doctors may recommend:
-
Close monitoring in early pregnancy
-
Progesterone support
-
Reassurance and emotional support
The prognosis is often better than expected.
Emotional Care Is Part of Treatment
Recurrent pregnancy loss is emotionally traumatic.
Couples may experience:
-
Anxiety with each positive test
-
Fear of attachment
-
Guilt
-
Blame
-
Isolation
Emotional support should be considered part of the treatment plan.
This may include:
-
Fertility counselling
-
Support groups
-
Couples therapy
-
Trauma-informed care
Emotional resilience improves treatment sustainability.
When Should Couples Seek Specialist Care?
Couples should seek evaluation if they have experienced:
-
Two or more miscarriages
-
Any second-trimester loss
-
A history of known genetic disorders
-
Repeated early pregnancy losses with no explanation
Early evaluation prevents unnecessary delays.
A Reassuring Reality
It is important to say clearly:
Recurrent pregnancy loss does not mean permanent infertility.
With proper diagnosis and targeted treatment:
-
Many couples achieve successful pregnancies.
-
Even couples with genetic challenges often succeed with advanced reproductive techniques.
-
Even unexplained cases often result in healthy births.
Final Thoughts
Recurrent pregnancy loss is one of the most emotionally painful reproductive experiences a couple can face.
But it is also one of the most medically manageable — when approached systematically.
The key steps are:
-
Comprehensive evaluation
-
Identifying the underlying cause
-
Targeted, evidence-based treatment
-
Emotional support throughout the journey
There is no universal solution — only personalised care.
If you or someone you love is experiencing recurrent pregnancy loss, know this:
You are not alone.
It is not automatically your fault.
And in many cases, there is still a very real path forward toward a healthy pregnancy.